Select a Topic
Proton therapy, or proton beam therapy or proton radiation, is an advanced cancer therapy that delivers a precise dose of high-energy proton radiation to the tumor, destroying cancer cells with less damage to surrounding healthy tissue.
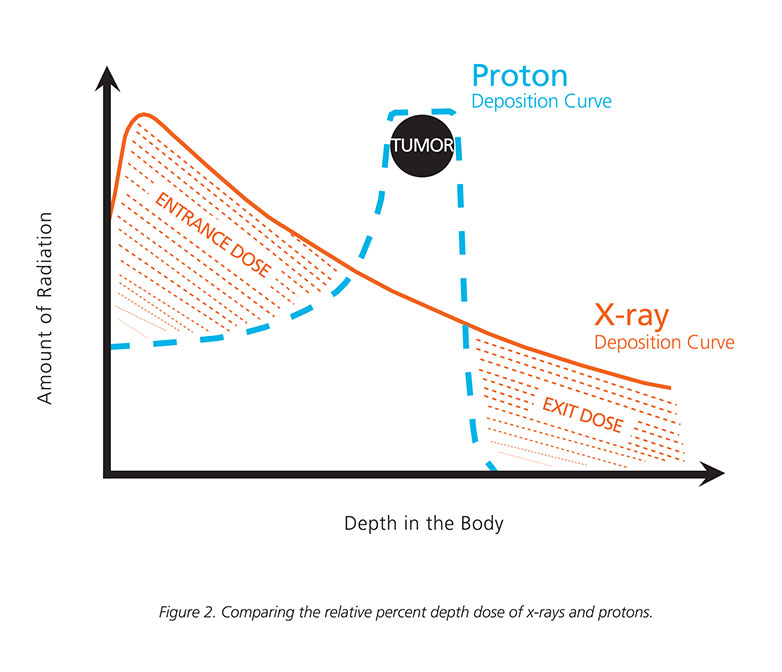
Proton therapy is an advanced form of radiation for cancer treatment that uses charged particles to precisely target the tumor. Unlike traditional radiation which uses X-rays, protons are charged particles with mass. Because protons have mass, the distance it travels can be predicted. It will only go as far as it is propelled and will stop, like a ball when it is pushed. Therefore, proton radiation therapy does not have an exit radiation dose. So, when protons enter the body from one side, they do not exit the body on the opposite side as X-rays do. The ability to stop radiation at a specific target results in lower incidences of side effects, both during and after treatment. The targeted dose of radiation is beneficial when the tumor is located in sensitive areas like the brain, head, neck, lung or prostate or in younger populations such as children and young adults. Read, "What is the difference between proton radiation and radiation therapy?"
Proton therapy is at least as effective as conventional X-ray radiation therapy but with fewer side effects. Many studies have demonstrated better cure rates with proton beam therapy than other radiation treatments. Also, proton therapy is the only radiation therapy option for some cancer diagnoses. Proton beam therapy is often used to treat tumors in sensitive areas of the body or to minimize radiation to surrounding organs or tissues. For example, a lymphoma patient may choose proton therapy treatment to also minimize radiation to the heart, lungs, esophagus, breasts and spinal cord.
Proton therapy is a more specialized form of radiation therapy and is used to spare radiation doses to radiosensitive structures. This means that proton therapy could be delivered to cancers anywhere in the body. The most common areas treated with proton beam therapy are prostate, breast, brain, head and neck, bones, eyes and pediatric-related tumors. At the Institute, we utilize proton therapy to treat some of the rarest tumors, including chordomas and chondrosarcomas.
In many cases, the side effects associated with proton therapy are fewer than those that come from traditional radiation. This is due to proton therapy's ability to effectively deliver radiation doses to the treatment site while doing considerably less damage to the healthy tissue surrounding the tumor. Your physician will review in detail with you any potential side effects prior to the start of your proton therapy treatments. Read our blog, "What are the side effects of proton beam therapy?"
To request more information, contact us today or call toll-free (877) 686-6009 and speak to our Patient Intake Services Department. They will answer general questions about proton therapy and help secure a consultation with a radiation oncologist. Prior to scheduling a patient's consultation visit, the UF Health Proton Therapy Institute will first work with the patient to collect a series of clinical reports and studies. Once we have this information, we will work with your schedule to quickly secure a consultation. During the consultation visit, one of our academic physicians will review your diagnosis and answer your questions about proton therapy and the best course of treatment for you.
No, proton therapy technology is not experimental, investigational or untested science. Proton therapy was FDA approved for use in the U.S. in 1988. Proton therapy has been around for almost 70 years; tens of thousands of patients have been treated, reimbursed by Medicare, Medicaid and many other private insurers. Reputable medical centers all over the world have embraced the technology and are building proton centers. The UF Health Proton Therapy Institute has treated more than 12,000 patients combined from the U.S. and 33 different countries. The center has published more than 400 proton-related publications that demonstrate the efficacy of the technology.
Proton therapy was only practiced at research facilities up until about 1990. Although it's been around much longer, proton therapy facilities are still limited in number. Even with dozens of proton centers in the U.S. today, fewer than 2% of all radiation treatments are proton therapy. Because of this, your doctor may not be completely familiar with the benefits of proton therapy. Ask your doctor if you may be a candidate, or contact us today to learn more.
Pencil beam scanning (PBS), also referred to as IMPT, is a delivery technique of proton therapy. Instead of using conventional beam-shaping equipment, such as brass, to shape the treatment, PBS utilizes magnets to steer the beam, creating a customized treatment delivery shape. Pencil beam scanning deposits the radiation dose, layer-by-layer, like a 3D printer. It conforms to the specific shape of a tumor and can be adjusted for intensity to achieve the desired dose distribution. Pencil beam scanning is ideal for complex cancers, in which the tumor is located near critical structures that can benefit more from a layer-by-layer dose.
Pencil beam scanning (PBS) has become the standard way proton therapy is delivered because of its improved high-dose radiation conformity. However, the Institute continues to offer both PBS and double-scatter proton therapy, so that patients can be assured the right proton delivery method is utilized for their care.
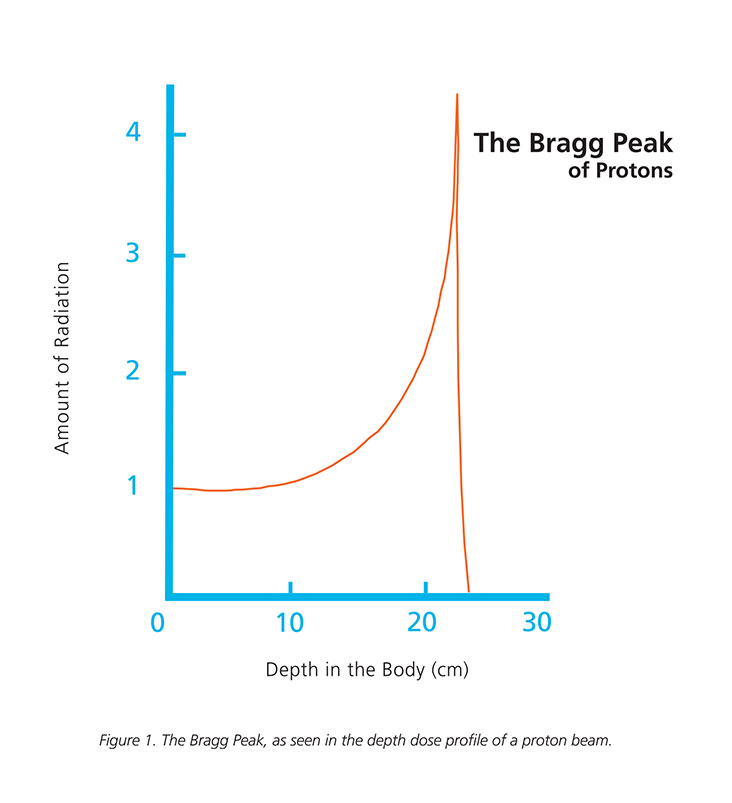
When protons stop, they release a burst of energy. This unique physical property is called the Bragg peak. Proton therapy, with its Bragg peak, allows for more precise dose distribution because the radiation stops in the body. There is no exit dose of radiation. This diagram illustrates the Bragg peak.
The UF Health Proton Therapy Institute offers patients the advantages of seeking cancer treatment at a nonprofit organization affiliated with the Southeast’s most comprehensive academic health center, UF Health. The UF Health Proton Therapy Institute is an integral part of the UF Health Cancer Center, one of a select group of prestigious cancer programs across the country to be designated an NCI-designated Cancer Center and the only NCI-designated Cancer Center backed by a state academic institute in FL. With over 300,000 treatments across more than 12,000 patients since 2006, the UF Health Proton Therapy Institute excels in staff experience, patient satisfaction and patient outcomes, driven by our dedicated team of highly skilled physicians and radiation oncology specialists. Experts from around the world in the field of proton radiation therapy reside at our institute to serve patients in an environment that's supportive and nurturing. In a recent study, 98% of patients surveyed said they would recommend the Institute to a friend or family member, and 99% reported excellent or good experiences during their daily treatments. Patient outcomes at the UF Health Proton Therapy center are also outstanding, showing favorable results in recent Hodgkin lymphoma, prostate and pediatric cancer post-treatment studies.
As the only nonprofit proton facility affiliated with a major academic health center in the region, the UF Health Proton Therapy Institute is a leader in cancer care.
Our state-of-the-art 108,000-square-foot radiation oncology facility combines the latest conventional X-ray radiation and proton therapy technology under one roof.
Our commitment to excellence has earned us numerous prestigious designations:
- Top five proton therapy facilities in the world: We proudly rank among the top facilities globally, serving a large number of patients.
- Cancer Center of Excellence: We are honored to be a two-time recipient of the State of Florida’s “Cancer Center of Excellence” designation.
- Accreditation from the American College of Radiology (ACR): We were the first proton beam facility in the Southeast to be accredited by the ACR, demonstrating our commitment to meeting the highest standards of quality and safety as certified by the ACR.
- National Cancer Institute Designation: We are proud to be part of the prestigious UF Health Cancer Center network, joining the ranks of the 72nd NCI-designated cancer center in the United States.
From the beginning of admission and the treatment process, patients at the UF Health Proton Therapy Institute get prompt and thorough answers and careful attention paid to all of their cancer treatment needs, including:
- Answers about proton therapy side effects
- Thorough explanation of the treatment process
- Guidance on financial and insurance matters
- Support groups and quality of life resources for patients and families
In the majority of cases, a physician referral is not necessary for treatment at our facility unless it is required by the patient's insurance provider. You can contact the Institute directly to find out more or schedule an appointment. Contact us today or call toll-free 877-686-6009 and speak to our Patient Intake Services Department.
No. The UF Health Proton Therapy Institute has appointments open and are available for new patients. It typically takes one to two weeks for medical records to be gathered, insurance to be verified and a consultation date to be set.
After an initial consultation with a UF Health Proton Therapy Institute radiation oncologist, patients take part in a simulation. Simulation involves gathering information to help pinpoint the exact size, shape and location of your tumor or lesion and surrounding critical structures using advanced imaging methods, such as magnetic resonance imaging (MRI), or CT (computed tomography) scanning. Customized immobilization devices will be created during simulation to position you during treatment, so proton therapy can be delivered precisely to the tumor every time. Learn more about treatment at the UF Health Proton Therapy Institute.
After a patient completes consultation and simulation, the patient is scheduled to begin treatment in approximately 5-10 business days. During the time between simulation and the start of treatment, a highly skilled team comprised of your radiation oncologist, dosimetrist and medical physicists will develop a customized treatment plan to maximize the treatment’s effectiveness and minimize potential side effects.
On the first day of treatment and all the remaining sessions, radiation therapists will replicate the patient’s simulation position, utilizing all the necessary immobilization devices. Once the radiation therapy team confirms the patient’s physical positioning matches the treatment planning prescription, only then will the patient receive treatment.
At the UF Health Proton Therapy Institute, a highly skilled and experienced team of radiation therapists takes great care to ensure each patient receives an accurate and precise proton therapy treatment. Our team's attention to detail and state-of-the-art technology enables us to deliver treatment with the utmost precision. To begin treatment, our team uses advanced image guidance to position the patient in the simulation position, a process that typically takes 10-15 minutes and involves accurately setting up the patient to ensure they are in the correct position for treatment. Once the patient is accurately positioned, our team delivers a non-invasive and pain-free proton treatment, which is typically brief, lasting only a few seconds or minutes. Our advanced beam delivery system allows us to target the tumor with precision, delivering radiation treatment from pre-planned locations to maximize the curative dose of radiation to the target while minimizing exposure to healthy tissues. Typically, each treatment session lasts 20-45 minutes each day, Monday – Friday.
External beam radiation therapy, including proton beam therapy, is noninvasive and pain-free; therefore, patients do not feel anything during treatment.
Proton therapy lends itself to reduced side effects both during and after treatment compared to other radiation treatment options. However, patients can experience side effects during treatment. When these side effects arise, your radiation oncologist and care team will help you manage those symptoms. Read, "What are the side effects of proton beam therapy?" to learn more.
Yes. Research on proton therapy continues to be conducted and reviewed by the medical and oncological community. In pursuit of the most accurate, effective practices and treatment, the UF Health Proton Therapy Institute has participated in more than 80 clinical trials and numerous peer-reviewed studies, including a 5-year study on prostate cancer outcomes. Learn more about clinical trials at the University of Florida Health Proton Therapy Institute.
When there is an indication to treat the regional lymph nodes, the heart and lungs are at higher risk of radiation exposure compared to treatment of the breast or chest wall alone. Proton therapy results in significantly reduced exposure of the heart and lungs to radiation while maintaining the high dose to the target regions. Thus, proton therapy for breast cancer can minimize the risk of side effects without compromising tumor control.
Typically, proton therapy treatment for prostate cancer is performed five days a week for six to eight weeks. Some patients may be eligible for a clinical trial that completes treatment in four weeks. Learn more about clinical trials at the UF Health Proton Therapy Institute.
Typically, treatment for other types of cancer with proton therapy last between four and eight weeks, for five days a week.
Yes, it is possible to have surgery following treatment for prostate cancer with proton therapy. It is important though to find a skilled surgeon that has experience in removing the prostate following radiation. While there are some recurrences with proton therapy, the percentage of these cases is very low.
Yes. Proton therapy is especially effective in treating childhood cancer. Proton therapy's ability to accurately target tumors in areas like the brain, head, neck, spinal cord and thoracic region helps to spare vital organs and surrounding healthy tissue, therefore allowing children to better tolerate and respond to treatment. As a child's body grows and develops, damage to healthy tissue and organs from radiation at a young age can cause growth abnormalities, reductions in IQ and the risk of tumor development as they grow. By reducing the radiation exposure to normal healthy tissue during the actual treatment process, proton therapy may reduce the risk of side effects and complications later in life. In addition to precisely targeting a child's tumor, the reduced risk of side effects during the actual treatment process make proton therapy an ideal choice for treating cancer in children.
Yes. At the Institute, patients, family members and caregivers can feel connected to a tight-knit community that involves group activities like new patient orientation tours, luncheons, group meetings and more. In addition, our social services team members are qualified, experienced professionals who assist the patient with a wide range of matters including the details of their stay, such as housing and transportation, but will also meet with the patient if there are psychological, financial or relationship issues. Click here to learn more about support for patients and families.
Only if your insurance requires it. If a referral is needed, our Referral Team will work to get the referral for you.
Proton therapy is covered by most major insurance carriers, and coverage continues to expand with major carriers based on the benefits of proton therapy treatment. Insurance coverage varies based on many factors, including cancer type, stage, and your specific insurance benefits. Our Financial Team will help you understand what your insurance will cover. Read, "Is proton therapy covered by my insurance."
Traditional Medicare is a federal program, so coverage for proton therapy does not vary from state to state. However, Medicare Advantage and secondary plans do vary. Often, these plans require pre-authorization before treatment can begin, and coverage varies from state to state.
You may need to check your coverage plan to determine if your proton treatment is covered or contact us for assistance.
Commercial insurance policies may or may not cover proton therapy according to their respective medical policy. Our team will review your benefits to determine if proton therapy is covered. If proton beam therapy coverage is not clearly defined, we will investigate directly with your payer. This process can take 3-5 business days.
We have treated patients from all over the United States and internationally. Coverage for proton therapy varies based on your specific diagnosis and insurance benefits and continues to expand with major carriers in the U.S.
You may need to check your coverage plan to determine if proton treatment will be covered out of state. Our coordinators will help guide you through the insurance process.
Prior authorization may be required before treatment can begin. If your insurance requires authorization, our team will handle the necessary paperwork and walk you through every step of the process.
In some cases, insurance coverage can be determined in as little as 24 hours, but may take as many as 2-3 weeks if delays arise.
It depends on your treatment plan. The cost varies based on many factors that impact your treatment plan, such as diagnosis, stage of disease and prescription of treatment dose.
We are here for you every step of the way, and will do everything we can to help you understand your treatment plan and costs.
There are self-pay options. The cost varies based on many factors that impact your treatment plan, such as diagnosis, stage of disease and prescription of treatment dose.
If this becomes a necessary option for you, our team will walk you through all your financial options.
Proton therapy is not experimental. However, many insurance companies consider proton therapy experimental, investigational or unproven treatment in their medical policies. We are constantly publishing new studies showing the value of proton therapy treatment, but insurance companies can be slow to update policies.
If your proton therapy is denied for this reason, our experienced appeals team will immediately start working to appeal the decision. At this time, you will also receive a cost estimate with the option to pay out-of-pocket. If you choose this option, you will begin treatment while we continue the appeal process. If your appeal is successful, we will ensure your reimbursement.
If an appeal is necessary, our team will file on your behalf. In most cases, our team is successful in overturning denied cases. Rest assured, we will continue to process your case until all levels of appeal allowed within your plan are exhausted. Read more about how we help with appeal process now.
SpaceOar is mostly made of water with an absorbable hydrogel, safely used in the body between the prostate and rectum to reduce rectal injury in men receiving radiation therapy for their prostate cancer. Eligibility for treatment with this system is determined by our radiation oncologist on a case-by-case basis. For further information on SpaceOar Hydrogel, please see www.spaceoar.com.
Varian TrueBeam is a conventional radiotherapy device that uses photons (X-rays) instead of protons to deliver radiation. It is equipped with Varian's RapidArc® radiotherapy technology, a system that delivers intensity modulated radiation therapy (IMRT) with speed and precision and allows for treatment techniques, such as stereotactic body radiation therapy (SBRT) and stereotactic radiosurgery (SRS).
Varian TrueBeam can be used to treat tumors that are in areas of the body that move, such as the lungs, head and neck and breast. It can also be used to treat cancer that has spread, or metastasized, if there are 10 or fewer lesions. Your radiation oncologist will review your case and determine which type of radiation therapy will achieve the optimal result.
Image-guided radiation therapy (IGRT) utilizes imaging during radiation therapy to improve the precision and accuracy of treatment delivery. This technology is featured in all our treatment rooms, both proton therapy and photon (X-ray) therapy. Read our blog, “Image-guided radiation therapy (IGRT) and radiation treatment accuracy” to learn more.


